Sibling Stem Cell Transplant Leads to Rare HIV Remission in ‘Oslo Patient’ : ScienceAlert
After receiving a stem cell transplant from his brother, a 63-year-old Norwegian man known as the “Oslo patient” has become one of only a handful of people to see their HIV (human immunodeficiency virus) go into long-term remission.
While HIV can now be controlled with medication that stops the virus from replicating, the virus remains in the body, rebounding when the drugs are stopped. So case studies like this one are invaluable for researchers working towards a full cure.
The Oslo man was given a bone marrow stem cell transplant to treat a rare type of blood cancer. Discovering at the last minute that his brother carried a rare genetic mutation previously shown to resist HIV, researchers led by a team from Oslo University Hospital closely tracked the operation’s impact on the virus.
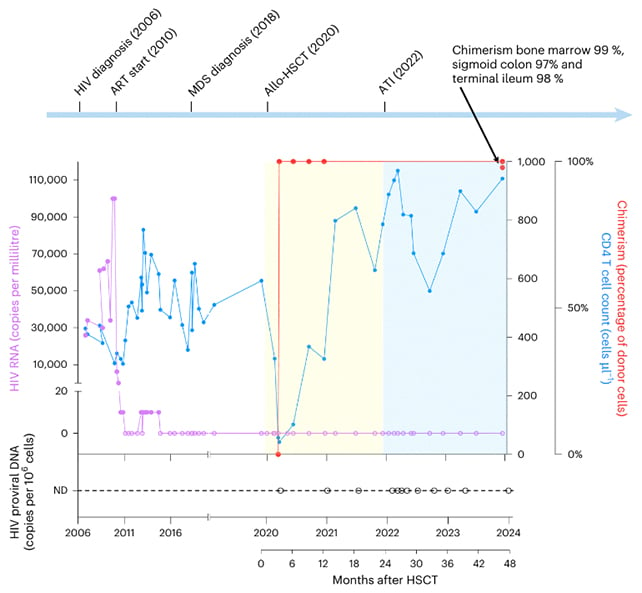
Four years after the transplant, called an allogeneic (donor) hematopoietic stem cell transplantation (HSCT), all traces of functioning HIV DNA were found to have been cleared in the treated individual.
He was able to stop his HIV medication two years after the HSCT, with still no evidence of viral rebound at 5 years post-HSCT.
“The case of the Oslo patient contributes valuable evidence to the existing knowledge base regarding HIV cure cases,” write the researchers in their published paper.
“Moreover, this and other studies on HIV cure enhance our understanding of HIV pathology, molecular mechanisms, and predictive biomarkers that may be of broader interest, extending beyond patients treated with allogeneic HSCT.”
The mutation carried in the brother’s genes, CCR5Δ32/Δ32, removes the CCR5 receptor on white blood cells that HIV normally uses as its entry point. It effectively makes the immune system impervious to HIV’s tricks.

Follow-up tests showed that the transplanted immune cells had indeed taken over. While some HIV fragments remained, they weren’t in a working state or in a state that could potentially be built up into a functioning virus again.
Though rare, cases like this have been recorded before. What makes this one particularly notable is that the gut was extensively tested and marked clear of functioning HIV DNA – and it’s here that the virus most likes to lurk in its dormant state, ready to emerge again.
The researchers also found that HIV antibodies in the Oslo patient declined, and T cells (part of the immune system) stopped responding to the HIV threat. It was as if the biological memory of the virus had faded, along with the virus itself.
“The absence of HIV-specific T cell responses in our data supports the hypothesis that such an absence correlates with sustained HIV remission,” write the researchers.
While this is encouraging news, bone marrow stem cell transplants like this are not a viable or practical option for a full HIV cure. These operations are risky reboots of the immune system, leaving patients very vulnerable to infection, and are performed only as a last resort when they can save lives.
As the researchers note, around 10-20 percent of those who undergo these transplants – for whatever reason – die within a year. Here, the Oslo patient experienced a severe reaction to the transplant, called graft-versus-host disease, which his body was ultimately able to overcome.
That immune system reaction (and the drugs used to clear it) may have been partially responsible for HIV being almost entirely wiped out, as well as for the new stem cells, the researchers say.
Related: Giant Study Reveals Why Some Viruses Hide Inside Your Body For Life
Further research can investigate this, and the team is keen to analyze data from all the rare ‘cure’ cases seen so far – to better understand what these patients can tell us about how HIV can be beaten.
“Moving forward, a critical step will be to compare existing cases of HIV cure to identify the most effective combination of biomarkers,” write the researchers.
“Conducting individual patient data meta-analyses is a logical next step, ideally followed by prospective sampling and new analyses that apply harmonized protocols in centralized laboratories.”
The research has been published in Nature Microbiology.



